Building community
Supporting families
Advancing research
We provide education, support, and community to patient-families navigating congenital lung malformations, like CPAM and BPS — while collaborating with clinicians to raise awareness and advance research in the field.
How we help
We provide a variety of connection and support options for patient-families, from texting with a parent to joining our friendly online drop-in group. And we share real life stories from families who have navigated these diagnoses and come out the other side.
We create clear, accurate and up-to-date materials, guides and tools on congenital lung malformations, always written by parents and carefully reviewed by medical experts. We also curate and share resources to navigate a lung malformation journey.
We support research and work alongside expert clinicians to learn from each other and break down barriers between medical teams and families and advance our understanding of these rare abnormalities.


CPAM Parents was founded in 2025, inspired by the connection between four moms who found each other after our babies were diagnosed with three different congenital lung malformations (CLMs): CPAM, BPS, and CBA.
We were struck by the amount of outdated and inaccurate information online and how little community existed for families navigating these rare conditions. So we decided to create it ourselves: a space that provides both up-to-date, expert-reviewed information alongside parent connection, support, and community.
Every week we now support families all over the world at every stage of a CLM journey, from diagnosis to birth to surgery and beyond. We partner with expert clinicians who help us create honest, accurate information that parents actually need. And we advocate for patient-families in medical communities and support research efforts.
Welcome to CPAM Parents. We’re so glad you’ve found us.
You don’t have to navigate this alone.


Latest articles
Latest Family Stories
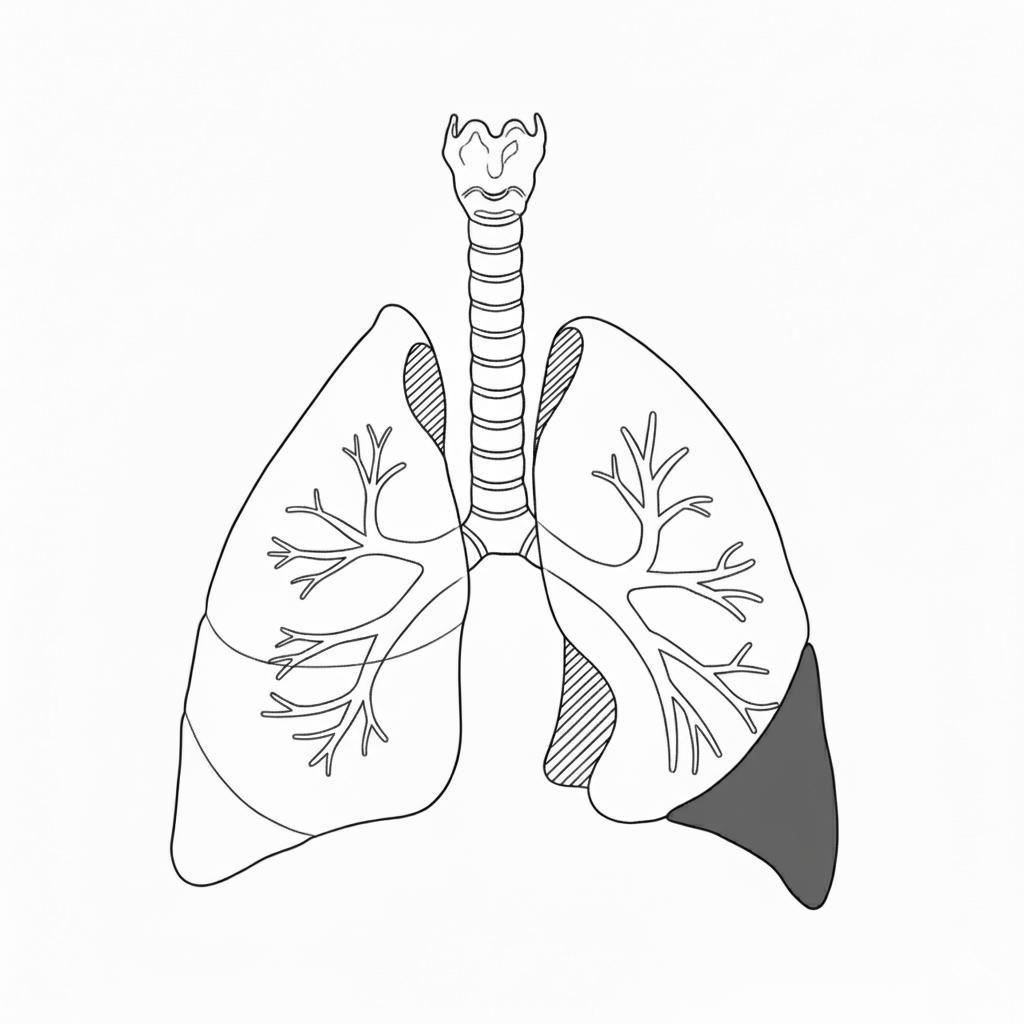
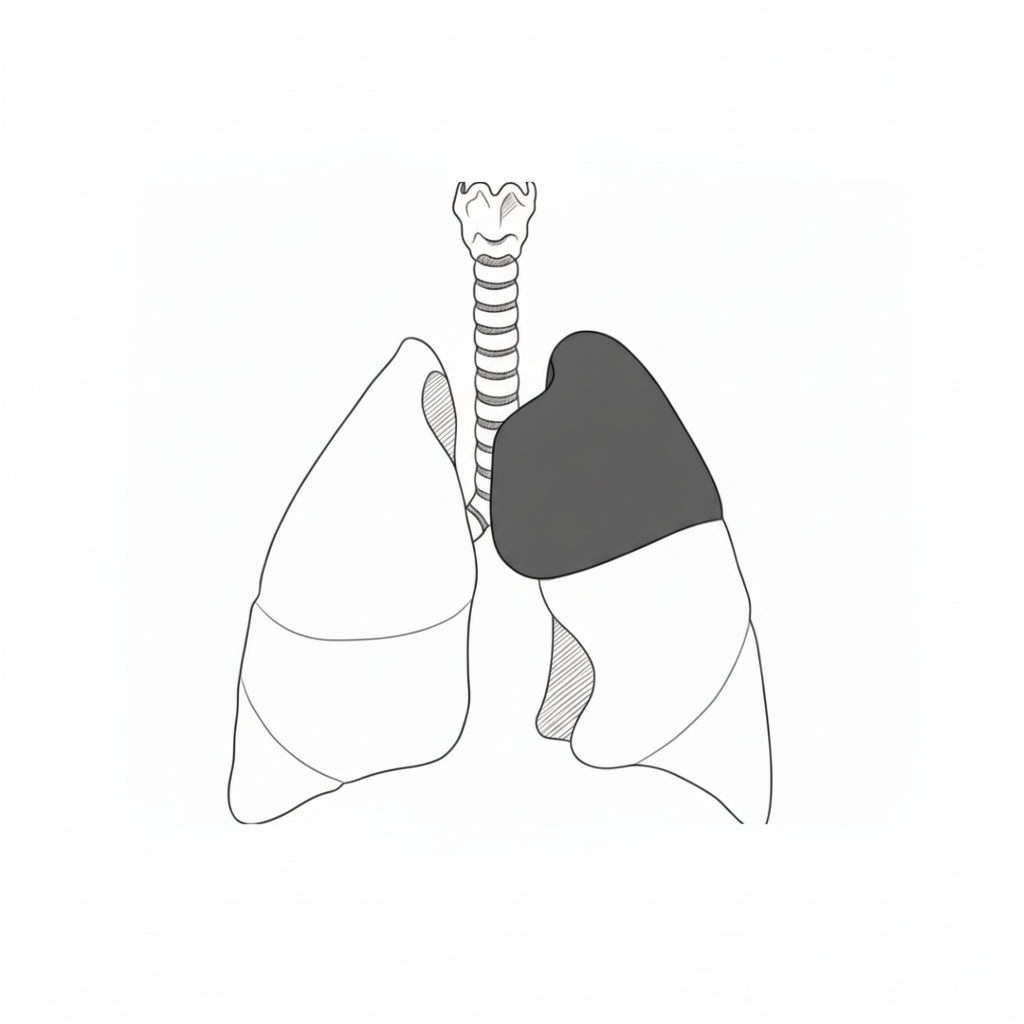
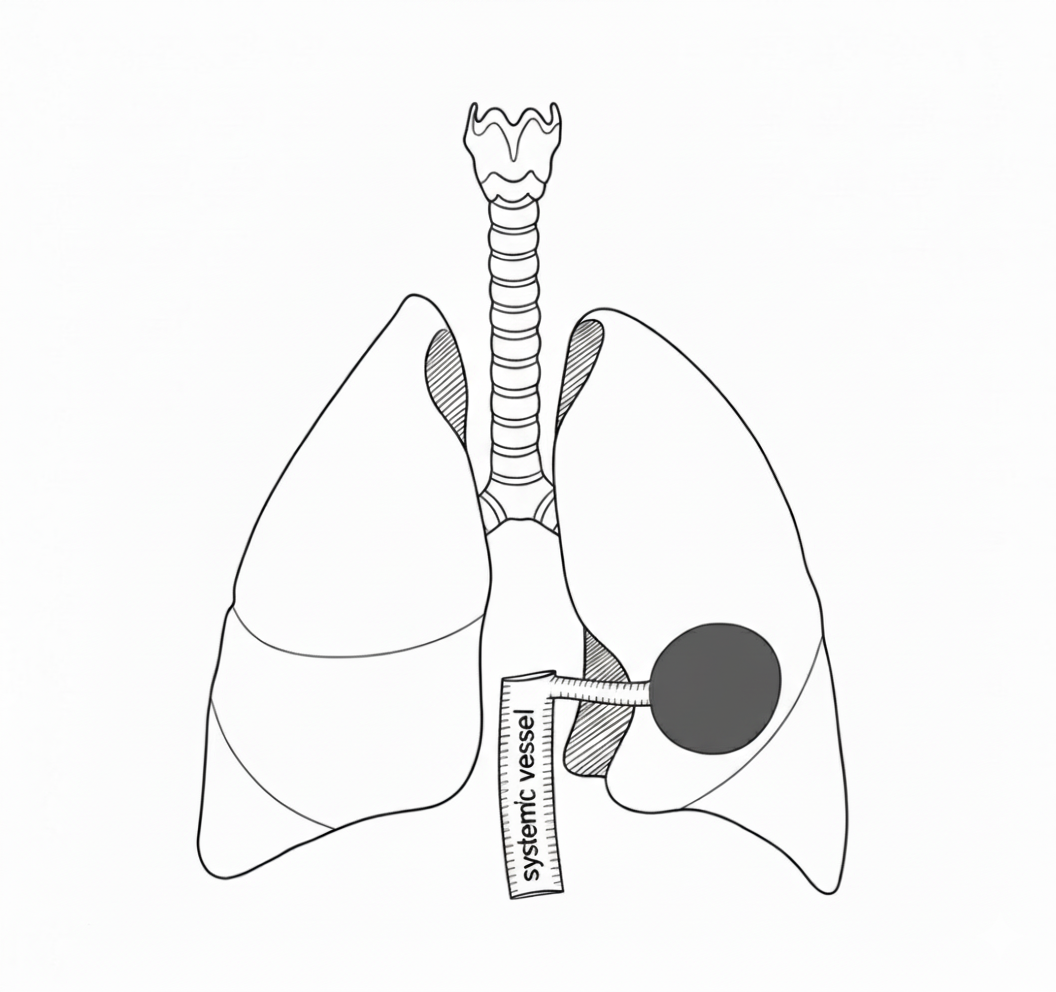
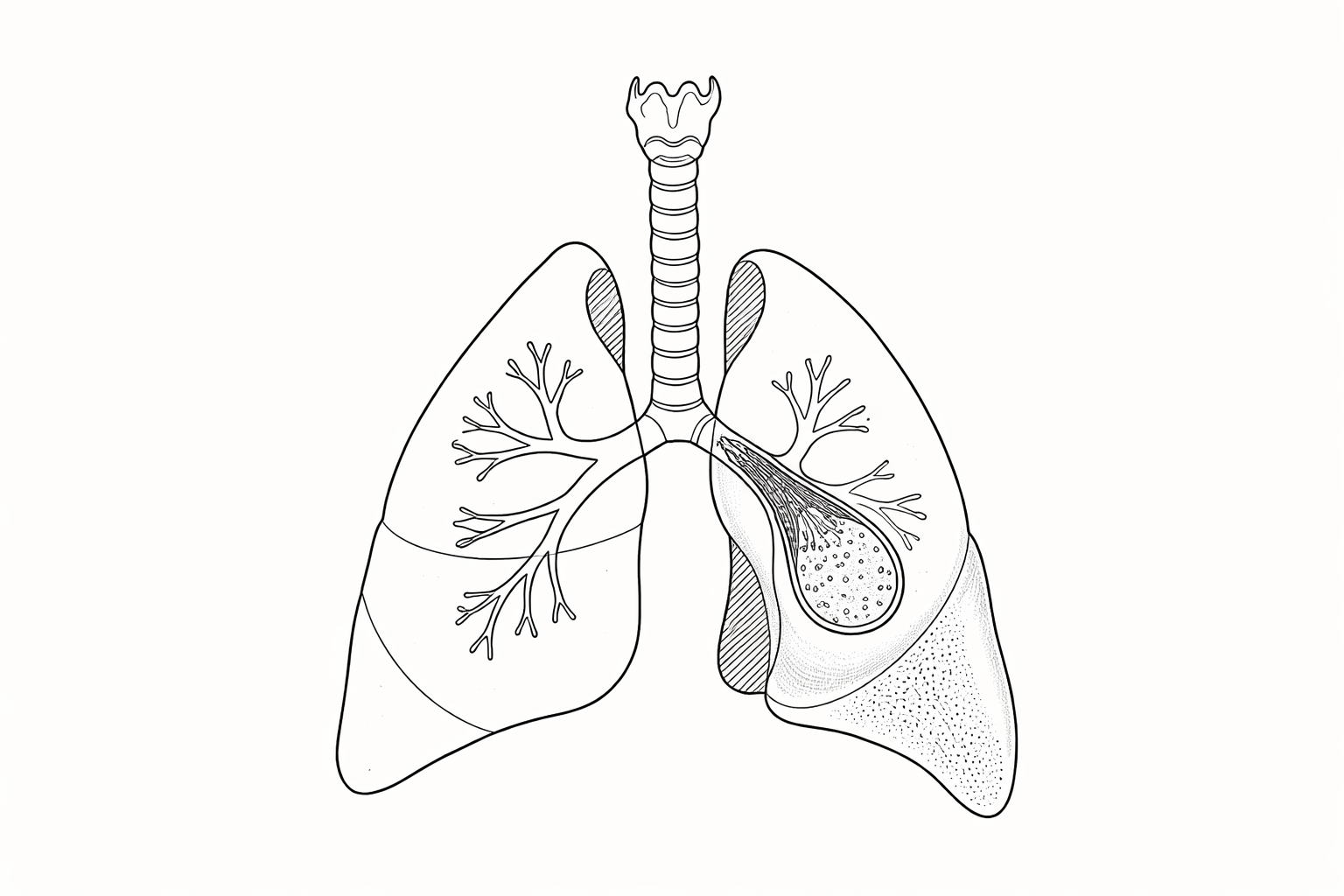
A congenital lung malformation (CLM) is a rare condition where part of a baby’s lungs did not develop normally during pregnancy.
In most cases the prognosis for babies born with a CLM is excellent. In about 20% of cases the lung malformation will cause serious complications prenatally and/or after birth.
There are different kinds of CLM: CPAM (congenital pulmonary airway malformation), BPS (bronchopulmonary sequestration), CBA (congenital bronchial atresia) and CLE/CLO (congenital lobar emphysema/overinflation).
Unlike many childhood conditions, there are currently no internationally agreed-upon guidelines for managing these rare and often complex abnormalities. Families are often faced with out-of-date or inaccurate information and conflicting advice.
We support patient-families from diagnosis through to surgery and beyond to improve the health, wellbeing, and care of babies with lung malformations and their parents.
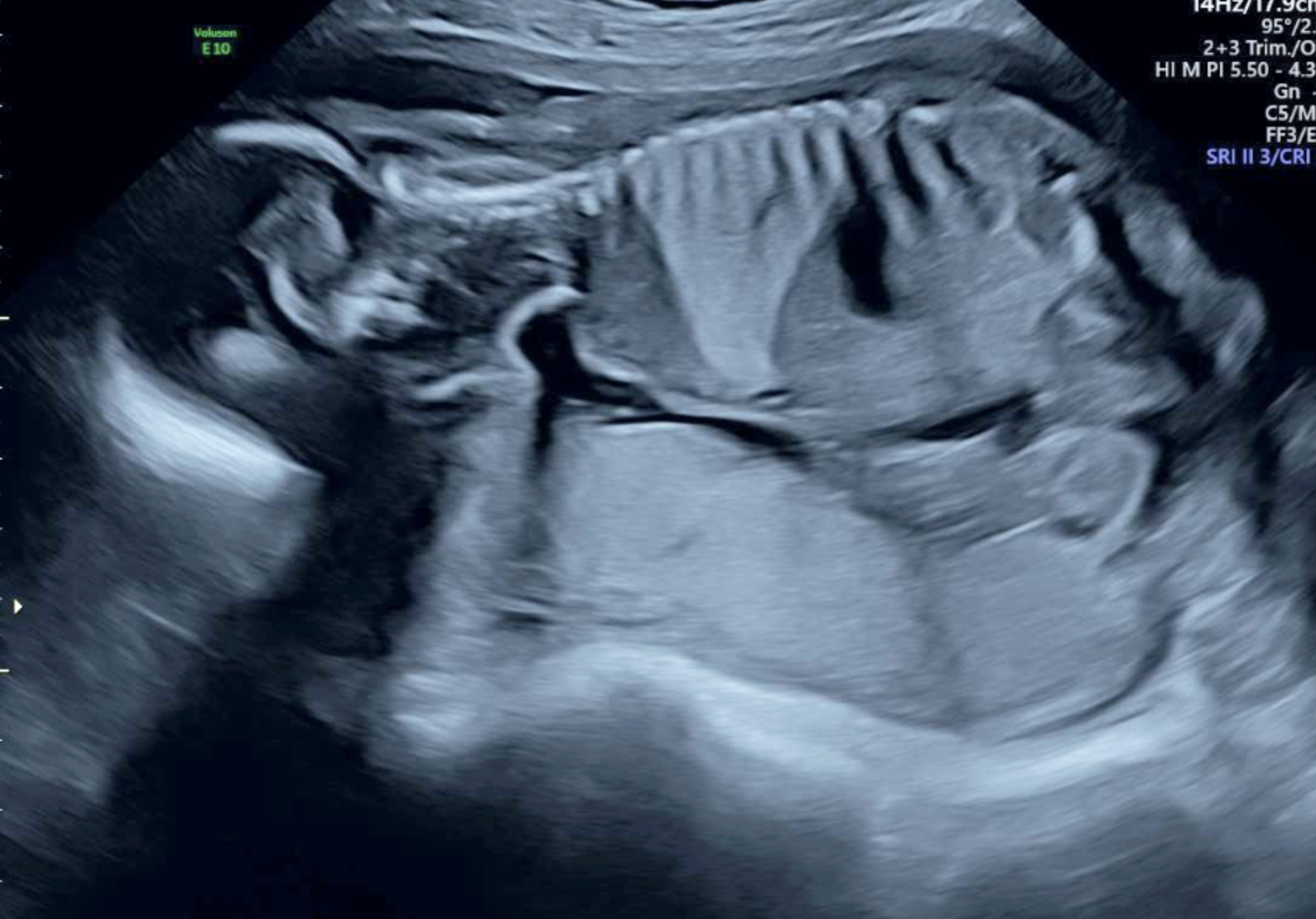


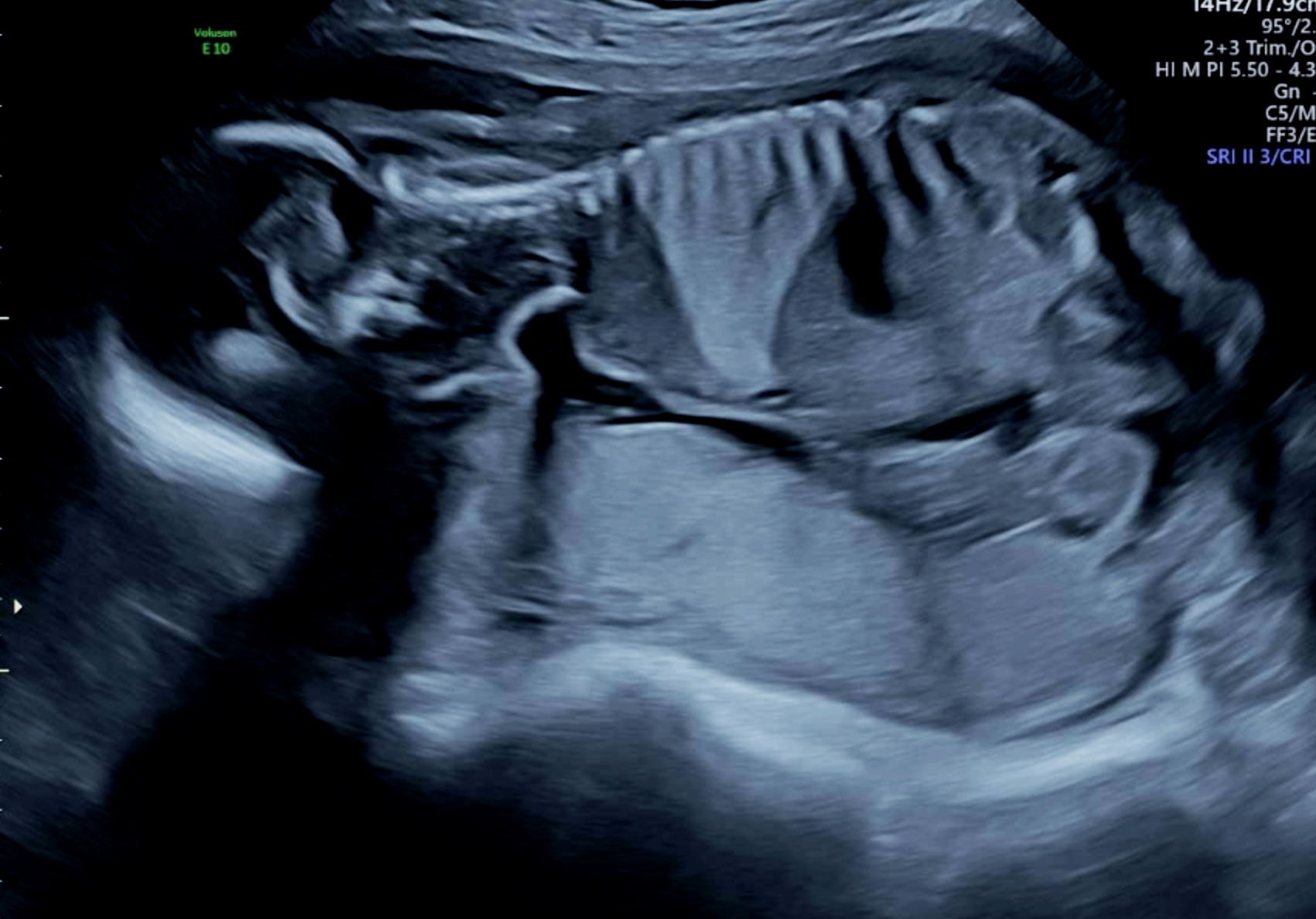
The bright wedge shape on this ultrasound is a lung malformation. This baby was diagnosed with a bronchopulmonary sequestration (BPS).

Parent Connections Program
Have a question about diagnosis, surgery, or anything in between? Want to talk to someone who has been there before?
Every week we provide clear and compassionate peer support for families navigating a congenital lung malformation — from diagnosis to surgery and beyond. You can contact us for a one-off consult or to be matched with a parent volunteer who has been through a similar diagnosis for ongoing support.
There are different ways you can connect with us.
Text: +1 (760) 650-2726
Email: talk@cpamparents.org
We will respond as soon as possible, normally within 24 hours. We provide peer support and practical guidance, we are not clinicians and we do not provide medical advice, but we can help you make sense of your diagnosis.
20%
Approximate number of CLM cases that are high-risk for prenatal or postnatal complications
90%
of babies with a lower-risk lung malformation will be able to breathe without support at birth
1 in 2,500
the estimated number of babies born with a lung malformation
70%
of lung malformations are currently diagnosed prenatally
Source: Shaun M. Kunisaki: Narrative review of congenital lung lesions, Translational Pediatrics 2021;10(5):1418-1431

Have you been through a lung malformation journey?
We would love to hear from you. We are always looking for compassionate volunteers to support newly diagnosed families: all experiences and all countries welcomed.